We’ve all been sitting in our homes for months now, and most days we hear something about how the vaccine to stop the spread of COVID-19 is just around the corner. There are actually over 160 vaccines in development, but two in particular are making the most headlines; one from Moderna Inc and another from University of Oxford. But what makes these two so special? And how close are they really to being available to you and me?
To summarize; There are a variety of vaccine types, and the biggest difference between them is how they use the pathogen in the vaccine. It can be a whole pathogen, just a piece of it or a newer method using the DNA or RNA of the pathogen. This new method, also known as a Nucleic Acid vaccine development, are what Moderna and University of Oxford are both creating.
Typically, for a vaccine to go from the lab to our bodies is a process that takes anywhere from seven to fifteen years. But we’re already seeing nucleic acid vaccines near the final stages of their development in a matter of months. This speediness is possible because these vaccines seem to be safer, cheaper, and easier to both handle and make. See, all a team needs to make this vaccine is the pathogen’s genetic code, not the actual virus itself. So in the case of COVID-19, SARS-CoV-2’s entire genome was sequenced in January 2020 and then uploaded to a public database for anyone to use. And then, the race was on.
Moderna made headlines early in the pandemic because they were one of the first to take this sequenced genome and combine it with their already developed mRNA technology called mRNA-1273. mRNA, or messenger RNA, is an instruction molecule that, well, does kind of what it sounds like; it instructs a cell on how to use that genetic code. So to get a lil technical, the team at Moderna isolated the part of SARS-CoV-2’s genome that makes the infamous “spike protein” that we see on coronaviruses. 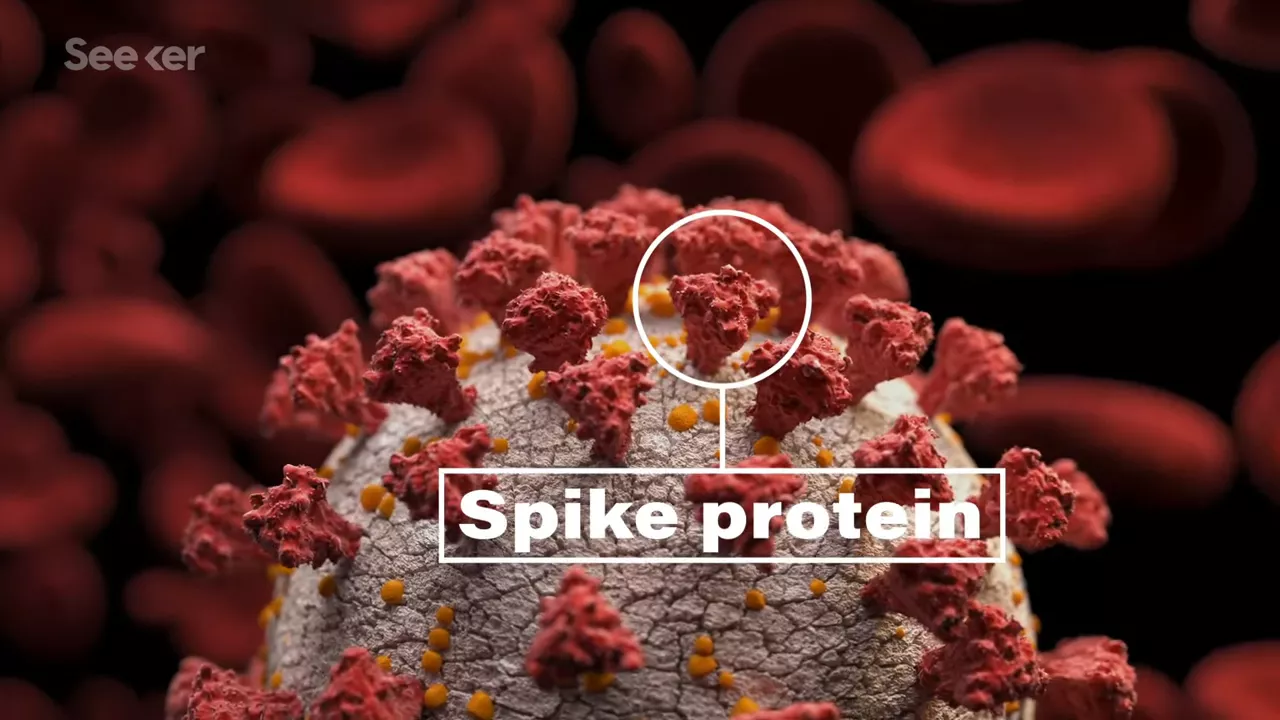 Then, they implanted that genetic code into an mRNA molecule. Aaand that’s the vaccine candidate!
Then, they implanted that genetic code into an mRNA molecule. Aaand that’s the vaccine candidate!
When injected into the human body, that vaccine will enter our cells, instructing them to use the viral code, and making our own cells produce their own “spike proteins”.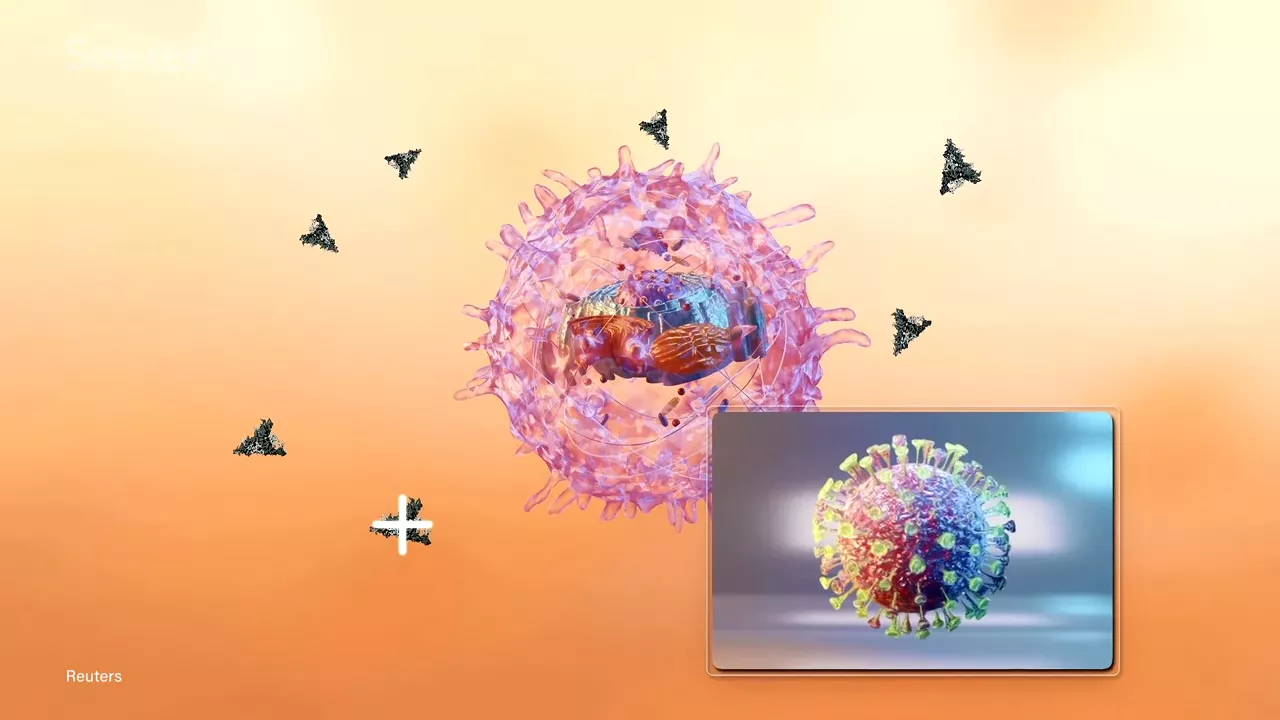 Our immune system can then identify those spike proteins as foreign stuff and begin doing what it does best to protect our body and produce antibodies to remember the infection for future protection
Our immune system can then identify those spike proteins as foreign stuff and begin doing what it does best to protect our body and produce antibodies to remember the infection for future protection
The best part about this technique, remember, is that the virus isn’t actually in our body. The vaccine is just mimicking what that would ‘look’ like to our immune system. So this mRNA method skips the usual time-intensive development process that’s required when to using live-viruses in a vaccine.
So great, we know how it works. When will we have it? Like all viable vaccines, these two promising candidates will have to pass the three major phases of development. With each phase of clinical trial, the amount of people the vaccine is tested on increases. As of July 27th, Moderna was the first U.S. vaccine candidate to enter a human clinical trial with 30,000 healthy participants who are at “high-risk” of contracting COVID. Many are coming from hotspot locations around the U.S. that have increased rates of infection, so scientists will be able see how the virus and the vaccine candidate interact in the real world. But waiting for that data to come back in and be processed will take a while, and it makes it a bit harder to get a reliable timeline on when we’ll finally get a vaccine for widespread use.
In Moderna’s case, they’re aiming to have preliminary data by the end of year, and they’re hoping to have their vaccine available sometime in 2021. Their manufacturing partner, a Swiss company named Lonza, plans on helping Moderna create up to one billion doses. That is, if it’s approved. And as far as the race goes, University of Oxford is not too far behind them.
Instead of an mRNA molecule, University of Oxford is using a weakened and modified version of a chimpanzee adenovirus vaccine vector. That’s basically a harmless virus that causes colds in chimps. Their vaccine is called the (ChAdOx1 nCoV-19) or AZD1222 and it also uses the genetic code for the coronavirus “spike protein”. But instead of placing it inside an mRNA molecule, the team placed these instructions inside the adenovirus. This induces a similar immune response to protect the body from future infections.
What makes ChAdOx1 so promising is that this method has been used before on another coronavirus called MERS, of which there was an outbreak in 2012. And unlike mRNA technology, the Chimpanzee adenovirus itself has already been studied for a number of years, and has already been genetically altered so that it’s impossible for it to grow in humans. That means it’s safe to give to children, the elderly, and those with pre-existing conditions like diabetes.
Oxford’s vaccine is already entering the final stages of their trial, which includes thousands of participants. The team estimates “a couple of months” for their data to come in, but again, the timeline is uncertain. But if everything goes to plan, the Australian government has already signed a letter of intent with distribution company AstraZeneca to secure 25 million doses of the vaccine. Because money is what’s really pushing these vaccines through the door.
The U.S.’s action plan, called “Operation Warp Speed”, is investing in both these candidates heavily, with almost $2.5 billion going to Moderna and $1.2 billion to AstraZeneca and University of Oxford. This is in order to reach Operation Warp Speed’s goal to distribute 300 million doses by January 2021. That’s an aggressive timeline that many doubts is even feasible. Not only would this be the fastest vaccine ever created, but also the first ever approved nucleic acid vaccine.
So as of right now, our best hopes are that either Moderna or Oxford’s vaccines will prove to be safe, and effective, and that one or both will be available and affordable for me and you. In terms of when this will all happen, the best we can optimistically say is maybe “sometime in 2021”. So until then, practice social distancing, wash your hands, wear your mask, and stay safe. For you and those you love.


No comments yet