Over the course of the pandemic so far, one trend that has emerged is that the health impacts of COVID-19 vary widely by race.
Although genetic factors have been considered by some as an underlying cause, it's clear from the overwhelming amount of public health data that something else is at play here.
If we take the U.S. as an example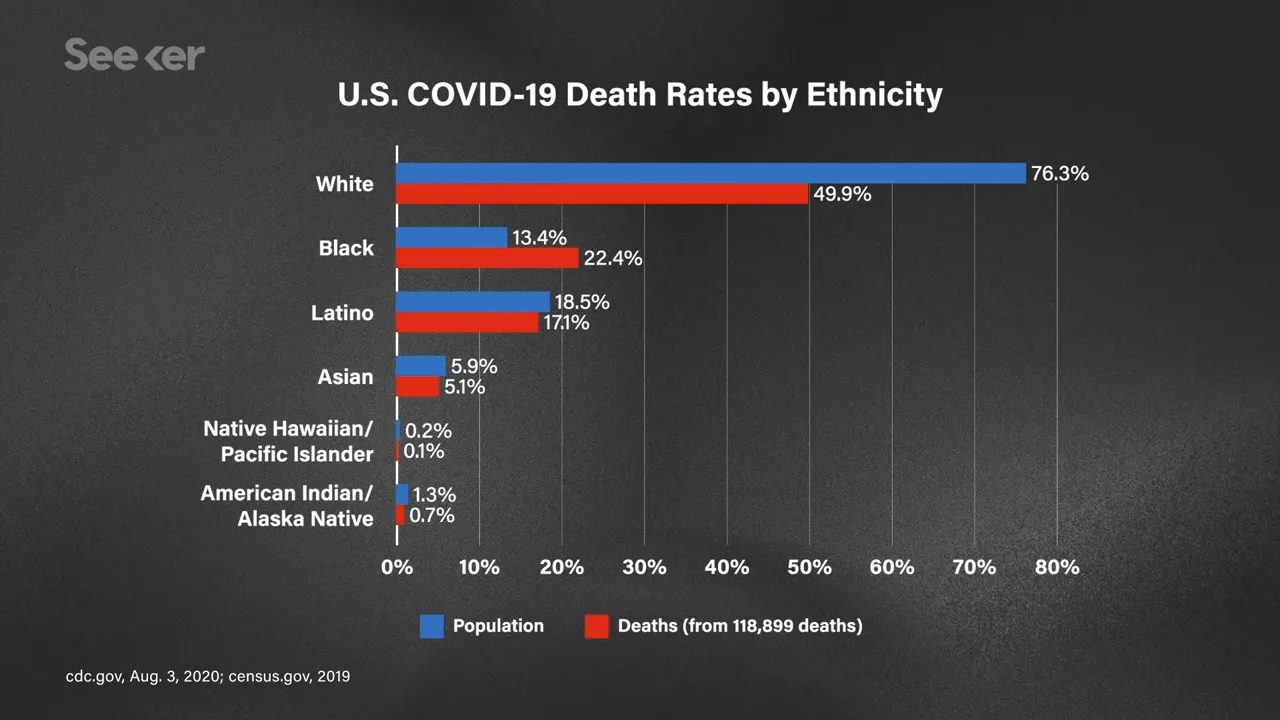 Overall, white people still make up the largest percentage of U.S. deaths from COVID-19, but white people also make up more than 76% of the total U.S. population. About 13% of the country’s population is Black, but Black people make up roughly 22% of the deaths from COVID and that means that Black people in the U.S. are dying at a rate that’s roughly double their population share.
Overall, white people still make up the largest percentage of U.S. deaths from COVID-19, but white people also make up more than 76% of the total U.S. population. About 13% of the country’s population is Black, but Black people make up roughly 22% of the deaths from COVID and that means that Black people in the U.S. are dying at a rate that’s roughly double their population share.
The disease is having a hugely disproportionate effect on Latinos and Asians compared to their population percentage. The Navajo nation had at one point the highest per capita rate of COVID-19 in the country.
So, before we get into what exactly is going on with COVID-19 in particular, we do need to clear a few things up. There are diseases that do have a genetic component that make them more common in certain groups, right, like sickle cell anemia, for example. Why is that?
When we think about things like sickle cell, that's a mutation that's protective against malaria. And so over time, people living in parts of the globe where malaria is a real threat and risk have sort of selected for that mutation in time. There is certainly much evidence to show that ancestry is probably the thing that we're short-cutting to when we talk about race. And so where people are from, their ancestors, there have been many, for example, adaptive mutations over time that are a response to the environment.
And there are genetic factors that play a role in how severely someone may be affected by COVID-19. That’s not only your genetic lottery when it comes to underlying conditions that might make it more difficult for you to handle or recover from this disease, but also specific genetic variations in cell surface proteins that the virus latches onto. But these genetic variables that I'm talking about here aren’t necessarily classifiable by race.
The conversation around COVID-19 and genetics, I think is an evolving one. And we will see what we learn regarding genetics and whether or not any genetic variance emerge as protective or as increasing risk. And then another layer is whether any of those are what we would refer to as ancestry informative marker associated variants. So you might see those variants, but they might be random. They might not actually be tied to ancestry at all. I think those are very important and exciting questions that we just haven't answered yet.
See, alleles are different ‘flavors’ of a gene, like how much and in what way that gene is expressed in an individual. For example, all humans have genes that code for hair, but what alleles we express determines how much, what color, what texture, etc. And this is an essential concept to grasp, because according to genetic research of allele makeup, there is no evidence that the groups we divide into different races have any kind of distinct unifying genetic identities.
Ultimately, there’s so much allelic variation across and within races that two people of European descent, for example, may be more genetically similar to a person of Asian descent than they are to each other. And many people may respond to this by saying, so what about skin color? But the superficial attributes that we used to classify each other by race, like skin, eyes, and hair, may only seem like such big divisions because they are so visible. But the genes that code for these characteristics are only a tiny portion of our genome, and they evolved independently from most of the rest of our genome, so they aren’t inherently linked to other genetic traits.
There may be a few exceptions to rules like this, like melanin expression in the skin affecting the likelihood of developing skin cancer, but these are pretty rare, and ultimately—humans share 99.9% of each other’s DNA.
So, if race doesn’t pre-determine our health on a genetic level in a vast majority of cases, then what accounts for the massive racial health disparities that we see in say, the U.S.?
Black infant mortality is more than two times higher than white infant mortality. 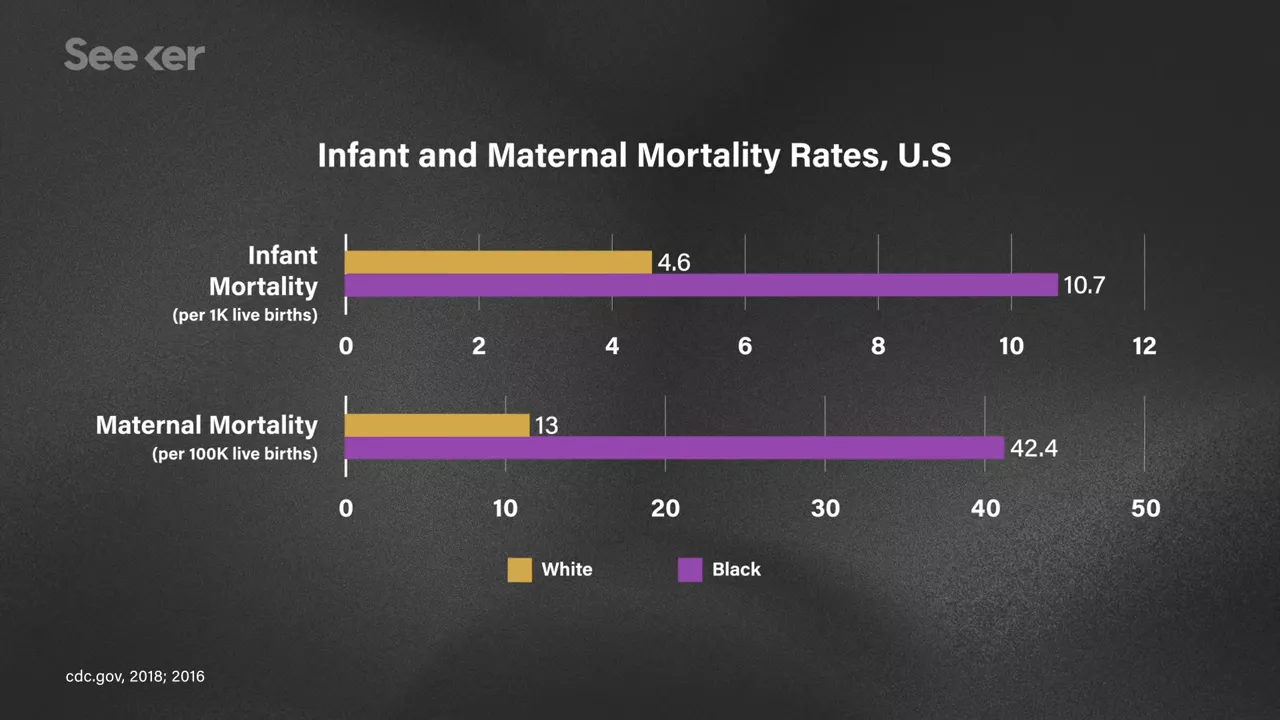 Pregnancy-related mortality is 3-4 times higher in Black populations than in white populations. Black patients experience significantly higher mortality rates for all kinds of surgeries and receive poorer treatment when it comes to pain management.
Pregnancy-related mortality is 3-4 times higher in Black populations than in white populations. Black patients experience significantly higher mortality rates for all kinds of surgeries and receive poorer treatment when it comes to pain management.
Similar trends in treatment disparities stand out between white populations and other non-white populations—like Latinos, indigenous communities, and Asian subgroups. And this is across huge swathes of medical treatments and patient outcomes. And all of this is evidence that even though race is not a genetically or scientifically valid concept, it’s still a pervasive social construct that does have real-world impacts on health.
We're having a reckoning now I think as a country with what has been a really intergenerational and systemic and structural disinvestment in communities of color. And all of that means in terms of denied access to opportunity and resources and how that manifests in social conditions that make the risk of infection higher for many black and brown individuals and neighborhoods, and then make the risk of severity that much higher too. And so, together I think it's important to state that we are learning a lot about this virus every day, but we will not discover at the end of the day that this is about biology or genetics when we look at the stark racial ethnic disparities.
The coronavirus pandemic in particular is the perfect lens through which we see that health is not so much about the actual bodies that we live in, but the social constructs that are imposed on those bodies.
Health is determined by your access to health care and education, what language you speak, how much money you make, whether you can afford to take time off of work to get seen by a doctor, whether you live alongside a lot of people or just a few, whether your job requires you to interact with a lot of people, and how your healthcare provider is going to treat you, literally.
And we can’t just consider these disparities in retrospect either: there are things we can actively do as we work toward future solutions to this pandemic, too.
I think it's important for us to do that work to make sure that we have a real diversity in all the things that we're doing around trials, experimental therapy, access to that, things like vaccine creation. Representation matters in this work that we're doing. And as we seek representation, we do it with the full understanding of knowledge that institutionally, we've earned mistrust from many people of color. Because of, frankly, our past — but also some of our present. So, we need to address that head on.
Now, in this article we’ve focused on statistics that are unique to the United States, but similar data from other countries shows that racial disparities in coronavirus infection and death rates exist in other places, too — like in the U.K., where South Asian and Black populations tend to be the hardest hit. And all of these investigations are actually kind of the beginning of the picture, because there are still numbers and stats missing, both for accurate case counts and for race of the affected patient.
So wherever you are in the world, you cannot consider the effects of any disease without also considering the underlying societal inequities at play. Much of our modern world has been built on a foundation of slavery and colonialism and to see the harmful, lingering echoes of those racist institutions in today’s society, like medicine, public health, all we have to do...is look at the data.


No comments yet